Drugs & Substance Abuse
The issue of substance misuse among children and adolescents remains a critical public health challenge. As of 2026, UK statistics show that while overall drug use among the youngest age groups has seen a general downward trend since the late 1990s, the complexity of the substances being used—and the speed at which some, like ketamine, are rising—demands renewed attention.
In the year ending March 2025, approximately 16,212 children (aged 17 and under) were in drug and alcohol treatment in England, a 13% increase from the previous year. Most of these young people (82%) began using substances before the age of 15.
- Common Substances of Concern
Introduction
Cannabis is the most frequently used illicit drug among young people. It is often consumed via “spliffs” (mixed with tobacco), bongs, or increasingly, in edible forms and vapes.
Facts & Figures
It remains the primary reason children seek treatment, accounting for 86% of all cases in 2025. Approximately 12.5% of 16–24-year-olds reported using it in the last year.
Warning Signs
Distinctive sweet, herbal smell; bloodshot eyes; increased appetite (“the munchies”); sudden lethargy or “spaced out” behavior.
Dangers
For the developing adolescent brain, cannabis is linked to a 3.3x higher risk of developing major depression. It can also trigger underlying psychotic disorders like schizophrenia.
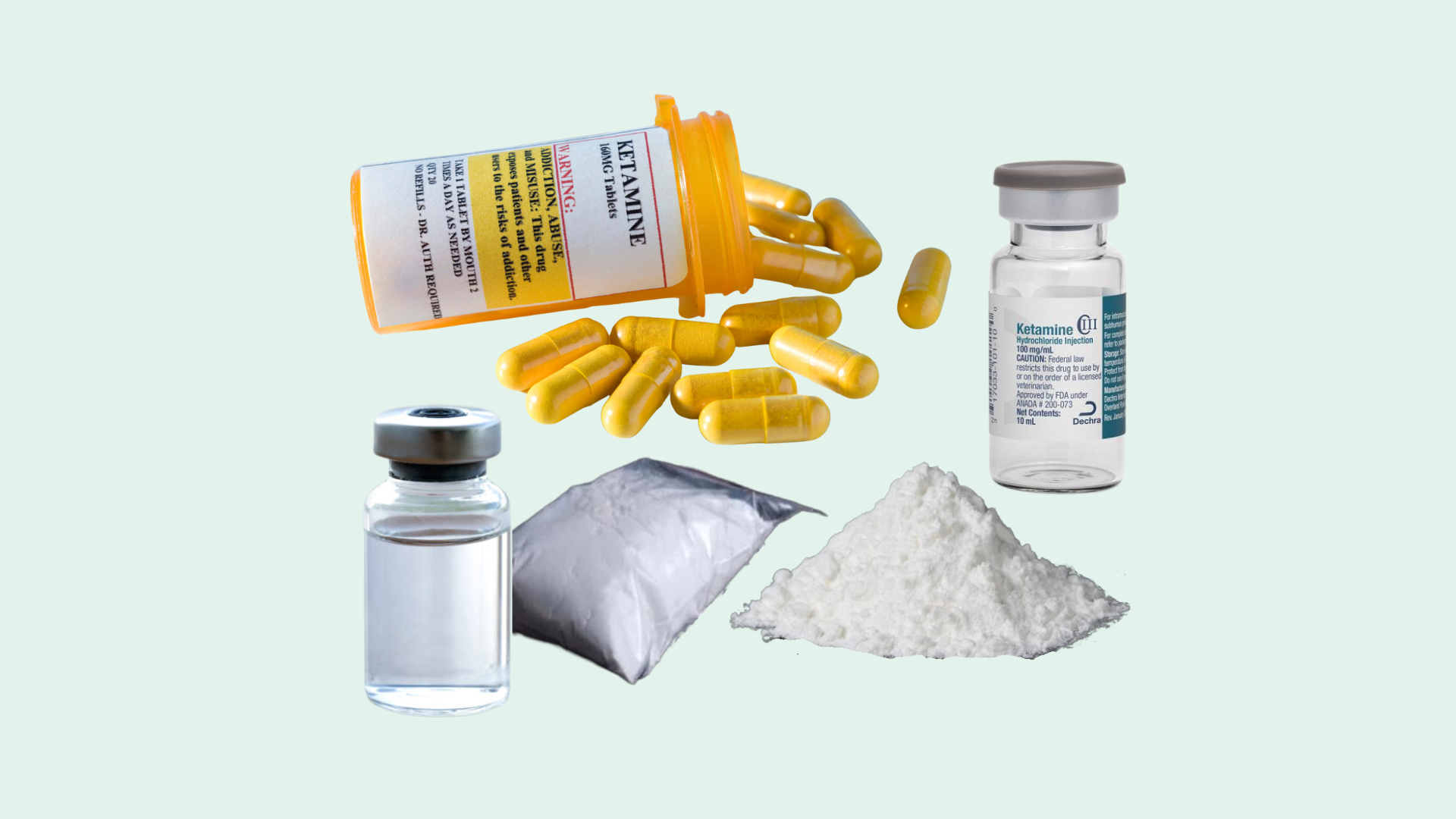
Introduction
Originally a dissociative anesthetic used in veterinary and human medicine, ketamine has seen a dramatic rise as a “party drug” among teenagers.
Facts & Figures
Treatment demand for ketamine has increased eight-fold since 2015. In 2025, more children reported problems with ketamine (9%) than with ecstasy for the first time.
Warning Signs
Slurred speech, “robotic” movements, numbness, and sudden confusion. A major physical sign is “K-cramps” (severe abdominal pain).
Dangers
It can cause irreparable bladder damage, leading to ketamine-induced cystitis where the bladder shrinks and becomes scarred, sometimes requiring surgical removal.
Introduction
Though often used interchangeably, “Ecstasy” usually refers to pill forms, while “MDMA” refers to the crystal or powder form. It is a synthetic drug that acts as both a stimulant and a hallucinogen.
Facts & Figures
Approximately 8% of children in treatment reported problems with ecstasy in 2025. Its use is heavily linked to the “nightlife” and festival scenes.
Warning Signs
Jaw clenching (bruxism), excessive sweating, dilated pupils, and a sudden, intense need to be physically close to or touch others.
Dangers
MDMA interferes with the body’s ability to regulate temperature, which can lead to hyperthermia (overheating) and organ failure.
Introduction
Cocaine is a powerful stimulant. In youth circles, powder cocaine is more prevalent, while crack cocaine use—though rarer in children—is associated with higher levels of exploitation.
Facts & Figures
Around 6% of children in treatment report problems with powder cocaine. In the 16–24 age group, about 3.8% used powder cocaine in the last year.
Warning Signs
Dilated pupils, extreme talkativeness, overconfidence, followed by “crashes” involving deep exhaustion and irritability. Frequent nosebleeds are common.
Dangers
High risk of cardiovascular failure (heart attacks), even in young people. Long-term use is linked to cocaine-induced psychosis in over 50% of users.
Introduction
Nitrous oxide is a colourless gas typically inhaled from balloons. It was classified as a Class C drug in the UK in late 2023.
Facts & Figures
Treatment for “solvent and inhalant” misuse increased from 3% to 6% over the last three years. Overall recreational use among 16–24-year-olds has dropped (from 3.3% to 1.3%) since its ban.
Warning Signs
Finding small silver pressurized canisters (“crackers”) or discarded balloons; unexplained dizziness or “fits of giggles”; numbness or tingling in hands and feet.
Dangers
Chronic use causes severe Vitamin B12 deficiency, leading to peripheral neuropathy—nerve damage that can cause permanent paralysis. Can cause sudden death through hypoxia.
Introduction
These are strong painkillers. Misuse among children often begins with “pill-sharing” from home medicine cabinets. In the UK, codeine-based linctus (syrup) is often mixed with soda to create “Lean.”
Facts & Figures
Around 1% of children in treatment specifically cite codeine as a problem substance. UK authorities are monitoring a slow but steady increase in “non-medical use” among adolescents.
Warning Signs
Extreme drowsiness (heavy eyelids), constricted “pinpoint” pupils, constipation, sudden “itchiness.” Missing medication from the family cabinet.
Dangers
The most immediate danger is respiratory depression—the drug tells the brain to stop breathing. Long-term use quickly leads to physical dependence and can act as a gateway to heroin use.

These are lab-made chemicals designed to mimic the effects of THC in cannabis. They are often sold as “THC vapes” to unsuspecting young people.
Facts & Figures
A 2024 study of vapes collected from UK schools found that 1 in 5 samples actually contained synthetic cannabinoids rather than nicotine or natural cannabis.
Warning Signs
Extreme agitation, “zombie-like” states (inability to move or speak), pale skin, profuse sweating, and sudden, unexplained aggression or terror.
Dangers
Unlike natural cannabis, “Spice” can cause seizures, heart attacks, and acute kidney injury. Very high risk of accidental overdose. Strongly linked to “Spice-induced psychosis.”
Signs of substance abuse
• Sudden changes in peer group
• Declining academic performance
• Changes in sleep patterns
• Unusual smells on clothing
• Secretive behaviour about whereabouts
• Unexplained money or possessions
• Physical signs: bloodshot eyes, dilated pupils, weight changes